Styes are incredibly painful! How long does it take to heal? An ophthalmologist breaks down treatment methods and prevention tips for styes.
Peeping at others while they bathe can cause styes or chalazia? How long do the symptoms last? Can they heal with self-applied ointment, or should one see an ophthalmologist for treatment? Many likely share these questions, especially the burning desire to know: once afflicted, how long will a stye or chalazion take to resolve? Before addressing these concerns, we must first understand the underlying mechanism.
Causes of Styes/Stye Formation
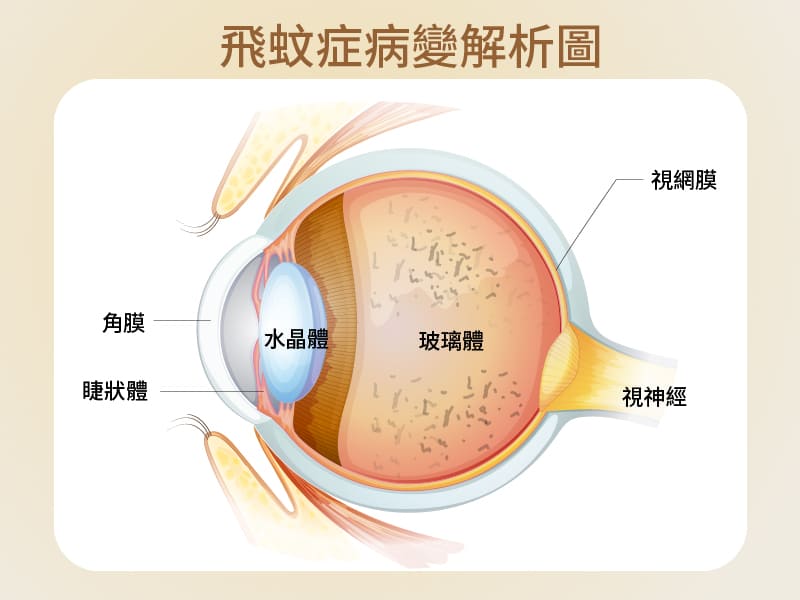
Stye, commonly known as a "pimple on the eyelid," is medically termed a "hordeolum." Styes typically develop near the meibomian glands and can cause eyelid redness and swelling. The primary cause of styes is excessive oil secretion from the meibomian glands, leading to gland blockage. This is often compounded by poor eye hygiene practices that allow bacterial infection to occur.
Additionally, if a patient frequently develops styes or chalazia, it may be due to eyelash follicles being blocked by mites. These tiny organisms can live at the base of eyelashes, and when they multiply excessively, they may cause inflammation and pus accumulation, ultimately forming styes or chalazia. So it's actually not caused by peeping on others while they bathe.
To prevent styes, daily eye care and hygiene are crucial, especially for those who frequently wear makeup. Thoroughly remove all makeup and avoid sharing cosmetics or makeup tools with others whenever possible. If styes recur frequently and persist for extended periods, consult an ophthalmologist to ensure proper management of the condition.
Characteristics and Symptoms of Styes/Styes
Styes/chalazia develop in different locations, corresponding to distinct names: "external hordeolum" and "internal hordeolum." External hordeolum forms in the superficial sebaceous glands near the eyelashes, while internal hordeolum develops within the deeper meibomian glands. Because the abscess forms on the inner side of the eyelid, the inflammation tends to persist longer.
In the early stages, symptoms may only include a slight sensation of something in the eye, which is not painful to the touch. Such symptoms typically resolve on their own with adequate rest and appropriate warm compresses. However, if the stye or chalazion becomes infected with bacteria, the following symptoms may appear:
Eye-picking syndrome
I. Mild Symptoms of Stye/Stye Infection
- Slight redness and swelling of the eyelids
- Mild itching and dandruff
- Foreign body sensation
- A scratching sensation when blinking
II. Severe Symptoms of Stye/Stye Infection
- The eyelids are noticeably swollen and enlarged, even affecting vision.
- Pain and slight warmth in the eyelids
- The sensation of a foreign object is very pronounced.
- Temporary astigmatism
If swelling or pain persists, consult an ophthalmologist immediately for treatment of a stye or chalazion.
How to treat a stye/eye boil?
Some patients attempting to treat styes or chalazia may try to puncture the affected area with a needle and then squeeze out the pus. However, this practice can lead to bacterial infection, causing the wound to become inflamed again or recur, or result in cellulitis, and may even trigger intracranial infection. Therefore, doctors do not encourage patients with styes or chalazia to use this method.If you discover you have a stye or chalazion, consult an ophthalmologist. Typically, when treating styes or chalazions, doctors will provide appropriate treatment recommendations based on the severity of the patient's condition.
I. Mild Stye/Stye Needle
For mild cases of styes or chalazia, maintaining good eye hygiene is key. At the onset, you may try warm compresses using a warm towel or a "hot egg" method to help the stye or chalazion resolve on its own.styes/pimples to subside naturally. To do this, boil an egg, wrap it in a gauze cloth without peeling it, and gently massage the eye area. Apply 4-5 times daily for 15 minutes each session. This melts and expels the blocked oil, reducing follicle obstruction. With this method, the stye/pimple will clear up in no time.
However, if you find the stye/pimple on your eye too painful, it is recommended to seek medical assistance first. The doctor will prescribe steroids or antibiotics based on the condition of the stye to help reduce inflammation and prevent infection.
II. Severe Stye/Eye Abscess
If a stye or chalazion persists with inflammation and shows no improvement after medication, the doctor may recommend a corticosteroid injection to reduce the swelling. However, this medication can cause whitening of the surrounding skin, making it less ideal for individuals with darker skin tones. In such cases, the doctor may suggest a minor surgical procedure to remove the stye or chalazion.This procedure is quite simple and leaves only a very small incision, resulting in no visible scar. If styes/chalazia frequently recur in the same area post-surgery, the doctor may send the tissue to a laboratory to rule out malignancy. However, lumps on the eyelid are usually benign and harmless.
How long does it take for a stye to heal?
As for how long it takes for a stye/hordeolum to improve, it depends on the severity of the patient's condition.Generally speaking, mild cases of styes/pink eye require patience and will improve within a few days as the swelling gradually subsides. Severe cases demand even more patience, with styes taking nearly two weeks to show improvement. If treated with patience, styes/pink eye often improve within days, and the duration of the condition can be shortened.
Whether you have a mild or severe case, the most important thing when dealing with a stye or chalazion is to seek medical attention promptly and be patient enough to wait a few days to see if it improves. Self-treatment of a stye or chalazion is absolutely not recommended, as this can cause further complications, leading to the stye or chalazion taking even longer to improve and heal. In such cases, recovery may take well over a month.
Are styes/pink eye contagious?
Generally speaking, styes or chalazia themselves are not contagious. However, if left untreated, they can lead to bacterial growth or demodex mite infestation. In such cases, they may spread to the other eye or to others through direct contact. Sharing towels, pillows, or cosmetics with an infected person increases the risk of transmission.
How long does it take for a stye/pink eye to heal, and how often does it recur?
Anyone who's had a stye or chalazion knows that feeling—not only is it extremely uncomfortable, but it can also directly affect your appearance. While it's not an emergency, it's definitely a major annoyance for some people, as styes and chalazions tend to recur frequently. To prevent recurrence, the key lies in maintaining good hygiene, adopting a healthy diet, and taking preventive measures.
- Practice good hygiene: Keep your hands clean, especially before touching your eyes. Avoid rubbing your eyes with your hands and refrain from using unclean towels to wipe your eyes.
- Healthy Sleep and Diet: Reduce late nights to allow your eyes sufficient rest, which helps regulate meibomian gland oil secretion effectively. Limit consumption of fried or spicy foods to lower the risk of inflammation in the body.
Preventive recurrence treatments are particularly effective for patients who frequently experience styes or chalazia, as these therapies eliminate parasites, reduce inflammation, and combat microorganisms. Take IPL (Intense Pulsed Light) as an example: IPL possesses photobiomodulation capabilities, effectively stimulating cellular mitochondria to promote cellular health. Treatments incorporating tetracycline or macrolide antibiotics aid in reducing inflammation and eliminating bacteria.
If not properly treated, styes or chalazia may persist for months and recur frequently, or lead to other more serious eye problems. Therefore, if you develop a stye or chalazion, the best course of action is to seek treatment from an ophthalmologist.
Why see an ophthalmologist?
Although styes are common, a doctor can accurately determine the type of stye you have, assess whether surgery is truly necessary, and select the most suitable incision location and technique. Postoperative follow-up is equally important. The doctor will provide detailed postoperative care instructions, schedule regular follow-up appointments to evaluate your recovery, and offer personalized advice to prevent recurrence. Only through this comprehensive treatment and follow-up can you truly resolve your stye issue completely.
💬 Book your eye exam now
Persistent stye? Schedule an appointment for a detailed assessment and treatment plan.
WhatsApp Inquiry About Styes#Sty Treatment #Sty #Sty Lancing #Sty #Sty Ointment