Many doctors use the eyes as a window to observe bodily ailments, especially in patients with chronic conditions. So, which diseases can affect the eyes?
Table of Contents
ToggleDiseases Affecting the Eyes
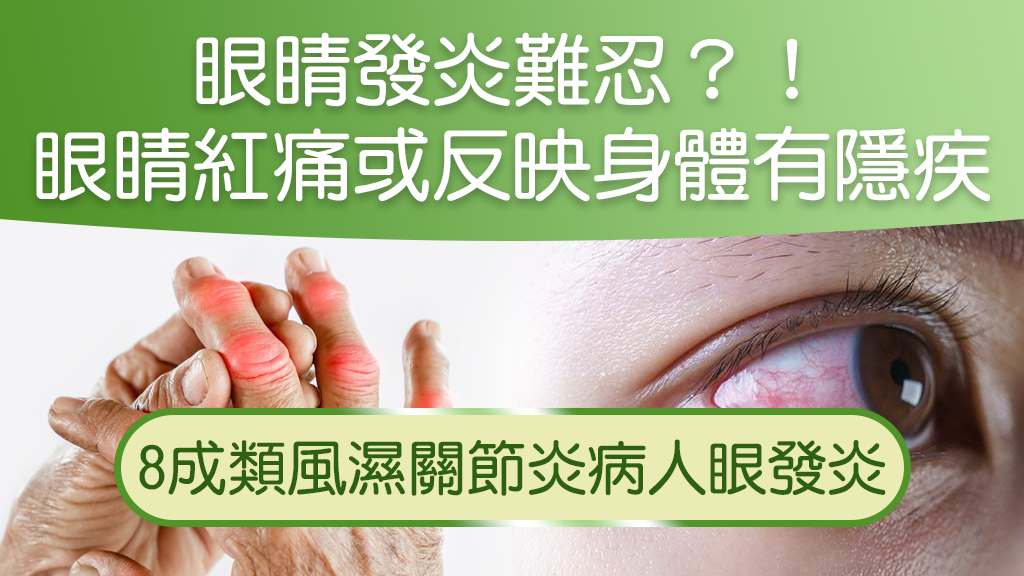
Eye pain, redness, and inflammation are common experiences among older adults. However, if these symptoms persist, we may become concerned about underlying health issues. One such concern is an autoimmune disorder, which can trigger inflammation throughout the body. The eyes are among the organs affected. If left unaddressed or untreated, this can lead to progressive vision loss and even the risk of blindness.
Symptoms and Treatment of Immune System Disorders
Immune system disorders can affect people of all ages, with the most common being rheumatoid arthritis, Sjögren's syndrome, ankylosing spondylitis, or lupus. Taking rheumatoid arthritis as an example, patients may experience lower back pain, hip joint pain, or inflammation symptoms that cause stiffness and soreness in the back upon waking. Due to inflammation, calcification may occur.Joints may fuse together, making it difficult to bend over or reach down to touch one's toes upon waking. Over time, this can significantly impair joint mobility. First-line treatment involves systemic therapy, typically prescribed by rheumatologists in the form of oral anti-inflammatory medications.
First-line treatment typically involves steroids. However, when high-dose steroids or prolonged therapy is required, second-line medications are generally used to mitigate steroid-related side effects. These second-line agents include biologics and immunosuppressants for long-term disease management.
Research indicates that eight out of ten patients will experience at least one episode of eye inflammation in their lifetime. Iritis is one such inflammatory condition that releases cells causing vision loss. These cells bind to proteins within the eyeball and accumulate in the anterior chamber angle, obstructing the drainage of aqueous humor. This leads to increased intraocular pressure, damaging the optic nerve and potentially resulting in glaucoma.
For treatment, blood tests are typically conducted to measure inflammatory markers, and X-rays are taken—such as chest X-rays or lumbar spine X-rays—to check for lung or spinal issues. If problems are found, medication is usually prescribed to control inflammation (specifically, anti-inflammatory steroid eye drops). Additionally, monitoring for side effects and complications is essential, with glaucoma medication used to manage intraocular pressure. Therefore, both ophthalmologists and rheumatologists collaborate to provide comprehensive care and treatment for the patient.
Medicine
Eye drops come in different types. Some are merely lubricating solutions that offer no therapeutic benefit and may even delay proper treatment. Others constrict blood vessels but do not control inflammation, potentially creating a false impression of ongoing improvement. Finally, if the treatment dosage is insufficient or the duration of use is inadequate, it can delay proper care and lead to irreversible damage to the eyes.
COVID-19
Conjunctivitis often accompanies respiratory infections such as influenza or viral colds, and it is also one of the symptoms of COVID-19. The most common symptom of conjunctivitis is redness and inflammation of the conjunctiva covering the white part of the eye. Research shows that among 30 COVID-19 patients examined during hospitalization, one exhibited conjunctivitis symptoms, indicating a close association.
To prevent COVID-19, first and foremost, we must wash our hands frequently with soap and water for at least 20 seconds. Additionally, we need to maintain a proper social distance of 1.5 meters and ensure adequate ventilation to protect ourselves from the virus.
Source: Topic