Causes, Symptoms, and Treatment Methods of Glaucoma
Glaucoma is a chronic eye disease known as the "silent thief of sight." It presents no warning signs, and early-stage glaucoma causes no significant pain or symptoms, making it difficult to detect. It is often only noticed when the patient's field of vision begins to narrow. However, by the time patients perceive this narrowing, their eyes have already suffered irreversible damage.According to figures from the Hong Kong Ophthalmological Society, 23% of patients who lose their vision become blind due to glaucoma. Individuals with hyperopia (farsightedness) and those over the age of 40 are considered high-risk groups for acute glaucoma.
Glaucoma results from elevated pressure within the eyeball, which gradually damages the anterior chamber, retina, and optic nerve fibers. However, some patients have intraocular pressure within the normal range (10-21 mmHg), yet their optic nerves remain vulnerable to pressure-induced damage, leading to narrowed vision.Early vision loss typically begins in the peripheral field, eventually leaving only the central portion intact. Without proper treatment, vision will progressively deteriorate and may be lost entirely.
Gain a deeper understanding of the underlying causes of glaucoma
Under healthy conditions, our eyes continuously produce a fluid called aqueous humor . To maintain healthyintraocular pressure, this fluid must drain out of the eye. Glaucoma occurs when intraocular pressure becomes too high, gradually damaging the optic nerve. However, some patients have normal intraocular pressure (10-21 mmHg) yet still experience optic nerve damage that narrows their vision.Early vision loss typically begins in the peripheral field, eventually leaving only the central portion intact. Without proper treatment, vision will progressively deteriorate and may be completely lost.
Ophthalmologist Tang Wenjie Explains Glaucoma Symptoms
Illustrated Guide to Glaucoma Symptoms

Types of Glaucoma
Glaucoma can be classified into different types based on its characteristics and causes. These include chronic glaucoma and acute glaucoma.
- Chronic Glaucoma
- In the early stages, there are no obvious symptoms, and patients may not notice any signs. As the disease progresses, the patient's field of vision gradually narrows, eventually leaving only central vision while peripheral vision is lost, resulting in what is known as "tunnel vision." If the condition continues to worsen, it may lead to complete blindness.
- Acute Glaucoma
- Sudden increases in intraocular pressure can cause noticeable symptoms such as blurred vision, seeing rainbow-colored halos around lights, eye redness, corneal clouding, severe eye pain, headache, and nausea or vomiting. If acute glaucoma is not treated promptly, it can lead to permanent vision loss within a single day.
Based on the underlying cause, glaucoma can be further classified into primary and secondary types.
- Primary Open-Angle Glaucoma
- No apparent cause, including open-angle glaucoma and angle-closure glaucoma
- Open-angle glaucoma refers to a condition where the anterior chamber angle remains open, yet elevated intraocular pressure leads to gradual damage of the optic nerve. In the early stages, most patients experience no noticeable symptoms or warning signs.
- Angle-closure glaucoma is characterized by an abnormally closed anterior chamber angle, which obstructs aqueous humor outflow and elevates intraocular pressure. If the angle closes slowly, the gradual increase in pressure may cause no symptoms in patients.
- No apparent cause, including open-angle glaucoma and angle-closure glaucoma
- Secondary glaucoma
- Elevated intraocular pressure caused by other conditions, such as mature cataracts, iritis, intraocular hemorrhage, tumors, trauma, postoperative complications, and inappropriate use of steroid medications. Glaucoma manifests in various forms, but early detection and prompt treatment are crucial for minimizing the risk of vision loss.
Symptoms of Different Types of Glaucoma
Want to know if you have glaucoma? In addition to comparing symptoms of different eye conditions, we can also delve deeper into the symptoms of various types of glaucoma.
Early-stage chronic open-angle glaucoma often presents with no obvious symptoms, but as the condition progresses, patients may gradually experience peripheral vision loss.
Early symptoms of acute angle-closure glaucoma may include eye pain, redness, blurred vision, eye swelling, and nausea or vomiting. An acute attack of angle-closure glaucoma can cause sudden, severe eye pain, headache, nausea or vomiting, blurred vision, and seeing halos around lights.
Causes and Risk Factors of Glaucoma
aged 40 or above
Advanced age is a significant risk factor for glaucoma. The prevalence of glaucoma increases exponentially with age. Individuals aged 60 and older have a sixfold higher risk of developing glaucoma.
Hypertension
Individuals with hypertension are twice as likely to develop normal-tension glaucoma compared to others. Hypertension damages the regulatory system of ocular blood circulation, leading to abnormal blood flow within the eye. Consequently, even when intraocular pressure remains within the normal range, hypertension accelerates the rate of optic nerve degeneration.
Diabetes
Research findings indicate that individuals with diabetes are twice as likely to develop glaucoma (primarily open-angle glaucoma) compared to those without diabetes.
suffer from cardiovascular disease
Individuals with cardiovascular disease have a significantly higher likelihood of developing glaucoma. While hyperlipidemia does not directly cause eye disease, research indicates a positive correlation between elevated blood lipid levels and increased intraocular pressure, thereby raising the risk of glaucoma.
Previously due to taking or applying steroids
Long-term steroid use can cause elevated intraocular pressure, leading to steroid-induced glaucoma. Prolonged steroid administration blocks the drainage channels of the eye, reducing aqueous humor outflow and consequently raising eye pressure. However, once steroid use is discontinued, intraocular pressure typically returns to normal levels in most patients.
Family History of Glaucoma
A family history of glaucoma carries a higher risk. Open-angle glaucoma is the most common form of hereditary glaucoma. If a first-degree relative has glaucoma, your risk of developing the disease increases by 4 to 9 times.
Eye injury
When the eye is struck by a hard object (especially in cases of blunt trauma), it may cause bleeding within ocular structures such as the iris, obstructing the flow of aqueous humor. This can lead to increased intraocular pressure, potentially triggering glaucoma.
Chronic Migraine
Chronic migraines are closely associated with glaucoma. Glaucoma generally falls into two forms: acute and chronic, with most migraine-inducing cases stemming from chronic glaucoma.On the other hand, migraines are sometimes mistakenly treated alongside acute angle-closure glaucoma. This occurs because the drainage channels in the anterior chamber of the eye become blocked within a short period, causing rapid increases in intraocular pressure. This may be accompanied by corneal edema, triggering severe headache symptoms. This condition is often misdiagnosed as a migraine, potentially delaying timely treatment for glaucoma.
Deep Hyperopia/Myopia
High myopia and hyperopia are also contributing factors to glaucoma. Hyperopic individuals are prone to angle-closure glaucoma, while high myopia is a risk factor for chronic open-angle glaucoma. Research further indicates that myopic eyes are more susceptible to elevated intraocular pressure. Individuals with myopia exceeding 500 diopters accompanied by increased intraocular pressure are particularly at risk for visual field narrowing.
Sleep Apnea
Recent literature studies indicate a relationship between sleep apnea and glaucoma. It is possible that patients experience oxygen deprivation during sleep, which may affect blood circulation around the eyeball, leading to optic nerve hypoxia and subsequent gradual vision deterioration.
Glaucoma Screening
Why is it important to have regular glaucoma screenings?
Glaucoma is a common eye disease that gradually damages the optic nerve and may ultimately lead to vision loss.However, early-stage chronic glaucoma often presents no obvious symptoms. Many patients only become aware of the condition once it has progressed to later stages. Once the optic nerve is damaged, the loss is irreversible. Therefore, regular glaucoma screenings are crucial for early detection and management. These examinations not only aid in early diagnosis and treatment but also help prevent vision loss.
Suitable candidates
- 18 years of age or older (especially those aged 40 or older)
- Individuals with high myopia (600 degrees or more)
- Diabetes patients
- There is a family history of glaucoma.
- The eye has sustained an injury.
- Suspected of having glaucoma
Comprehensive Glaucoma Examination Scope
1. Medical history taking and medical record review
Understanding the symptoms of vision problems and eye diseases
2. Visual acuity and refractive error examination
Through various procedures and instruments, we accurately assess patients' visual acuity, including myopia, hyperopia, astigmatism, and presbyopia.
3. Intraocular Pressure Measurement
Intraocular pressure is one of the primary indicators for glaucoma. Doctors typically measure it using a non-contact tonometer or an instrument that applies gentle pressure. This process is generally painless and can be performed at an ophthalmology clinic.
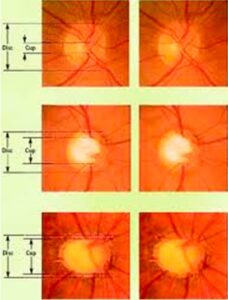
4. Optic Nerve Examination
In the diagnosis of glaucoma, optical coherence tomography (OCT) plays a crucial role. This non-invasive optical diagnostic technique allows physicians to examine the eye using high-resolution optical analysis to identify signs of optic nerve damage. Through advanced instrumentation, it enables a more detailed assessment of optic nerve health and provides a comprehensive evaluation for early glaucoma detection.Early detection of optic nerve damage enables the formulation of appropriate treatment plans.
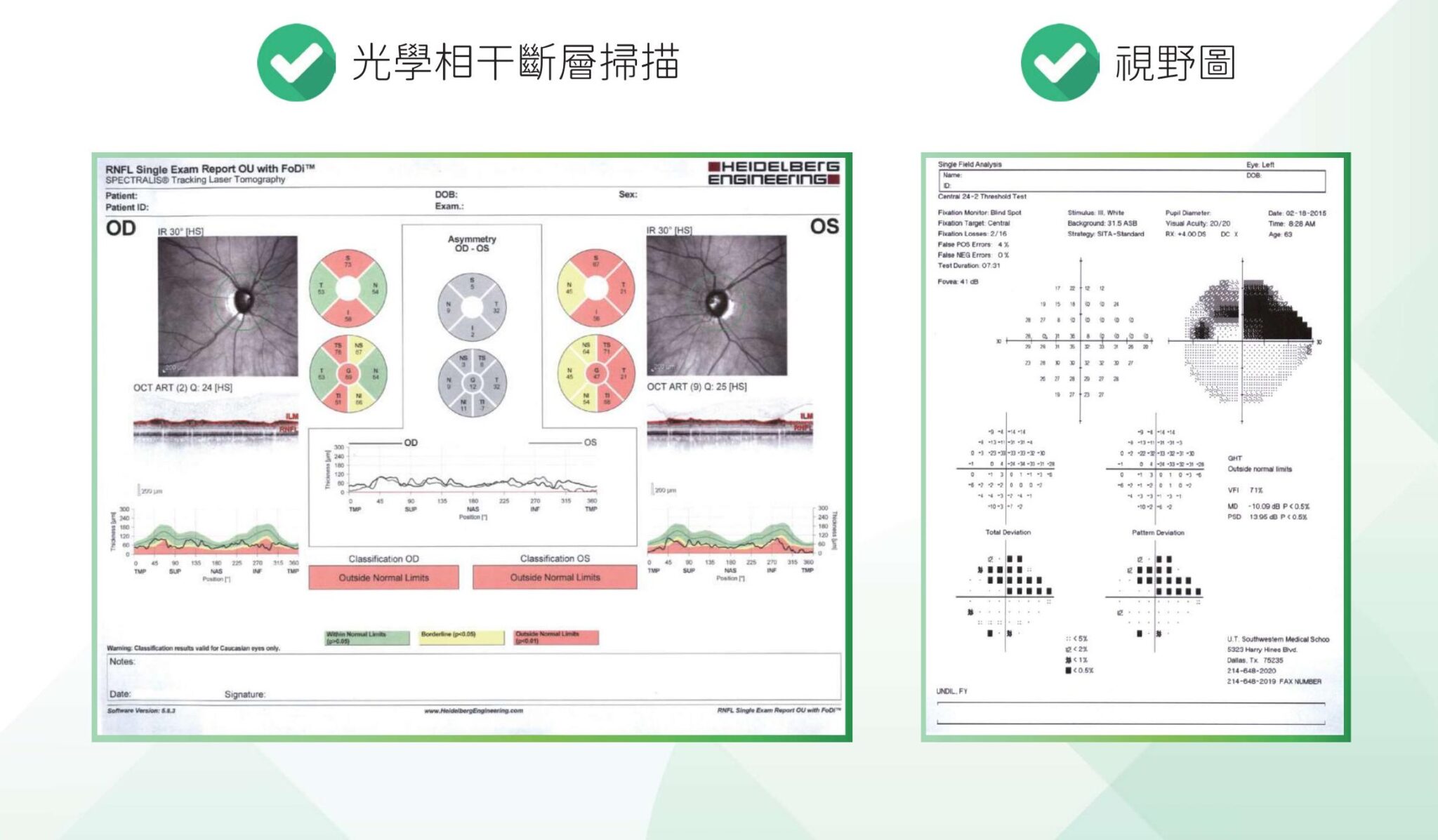
5. Visual Field Examination
Visual field testing helps doctors assess the integrity of the visual field and identify any potential defects. This examination is typically performed using an automated perimetry device, where the patient focuses on a specific point while detecting changes in the brightness of light spots in various directions. This helps doctors determine whether the visual field has been compromised.
6. Mirror examination
Ophthalmoscopy involves using lenses to evaluate the structures of the anterior and posterior segments of the eye. Through this examination, doctors can assess the health of areas such as the iris, lens, and retina. This procedure provides crucial information about the internal structures of the eye.
7. Analysis and Construction
Glaucoma Treatment Methods
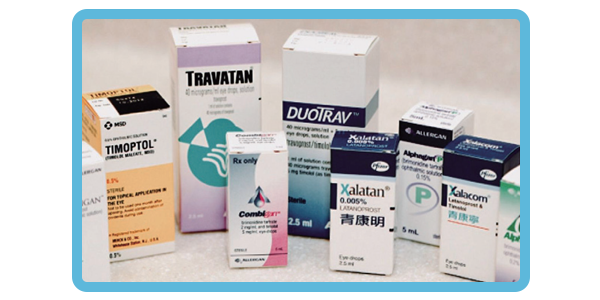
Prescription eye drops are one of the common treatments for glaucoma. These drops help control intraocular pressure to an appropriate target range, protecting the optic nerve tissue and reducing further vision loss. As a non-invasive treatment, eye drops carry a lower risk of side effects and are safer than laser or surgical interventions. Many glaucoma medications now come in combination formulations, allowing patients to manage their condition with just one drop per day.
If glaucoma cannot be controlled with medication, patients may consider laser and surgical treatments such as trabeculectomy, drainage procedures, tube shunt implantation, cyclophotocoagulation or cryotherapy, argon laser peripheral iridoplasty, and minimally invasive glaucoma surgery.
- Trabeculectomy is a surgical procedure that removes part of the trabecular meshwork to enhance aqueous humor drainage, thereby reducing intraocular pressure.
- Drainage surgery involves creating a new drainage channel within the eye to facilitate the outflow of aqueous humor.
- Tubal implantation involves inserting a drainage tube into the eye to guide the outflow of aqueous humor.
- Ciliary body photocoagulation or cryotherapy involves using laser or cryogenic techniques to destroy ciliary body tissue, thereby reducing aqueous humor production and lowering intraocular pressure.
- Argon laser peripheral iridotomy uses argon laser to enlarge the aqueous humor outflow channels, thereby increasing the volume of aqueous humor drained.
A New Option for Patients with Mild to Moderate Glaucoma: The Latest Glaucoma Treatment Approach
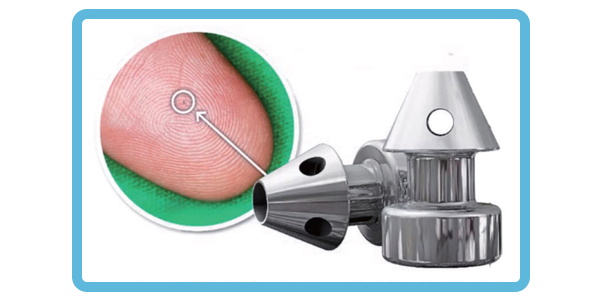
In recent years, minimally invasive glaucoma surgery (MIGS) has been introduced. Compared to traditional glaucoma surgery, it is less invasive, thereby reducing potential complications and offering a new option for patients with mild to moderate glaucoma. MIGS provides greater safety, faster recovery times, and reduces the burden of glaucoma medication for patients.
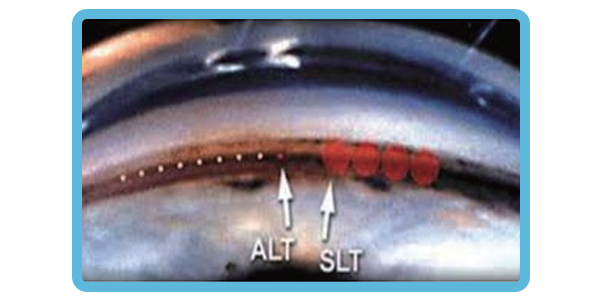
Selective Laser Trabeculoplasty (SLT) is an in-office procedure that reduces intraocular pressure in glaucoma patients. The laser is directed through a special lens onto the eye's drainage system, where it stimulates biochemical changes that improve the outflow of aqueous humor from the eye. Due to its favorable risk-benefit profile, SLT offers an early treatment option in glaucoma management strategies, including as a primary treatment approach.
Studies comparing SLT and eye drops as primary therapies found similar treatment outcomes between the two groups. Although some patients still required eye drops after SLT, they needed fewer drops to control their glaucoma.
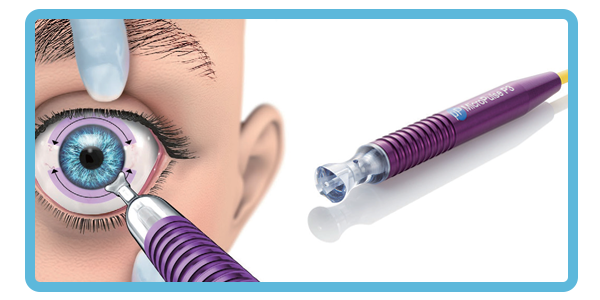
The MicroPulse® P3 Glaucoma Device (MP3) delivers treatment via the CYCLO G6 Glaucoma Laser System, utilizing non-pulsed, repeatable, and predictable MicroPulse technology to provide innovative circumciliary photocoagulation. This procedure disrupts ciliary body tissue, reducing aqueous humor production and thereby lowering intraocular pressure.
Frequently Asked Questions About Glaucoma
What foods can help prevent glaucoma?
It is recommended to increase intake of vegetables and fruits rich in vitamins, minerals, and antioxidant nutrients, such as kale, carrots, and peaches. Additionally, consuming nitrogen-rich foods like dark leafy greens may also help reduce the risk of glaucoma.
How long after being diagnosed with glaucoma will I go blind?
Glaucoma does not necessarily lead to blindness; with consistent treatment, the condition can be effectively managed. The probability of blindness resulting from glaucoma ranges between 10% and 25%. In cases of acute glaucoma, if left untreated, patients may face the risk of blindness within days.
Chronic glaucoma typically presents no obvious symptoms in its early stages. When issues such as blurred vision, difficulty seeing objects clearly at certain angles, or tripping on stairs arise, it usually indicates that glaucoma has progressed to an advanced stage. Patients may face the risk of blindness within 3 to 5 years.
Can glaucoma be cured?
Glaucoma currently has no complete cure, but with early and accurate diagnosis and treatment, along with close cooperation with an ophthalmologist, it is possible to maintain the best possible condition of the eyes.
How can glaucoma be detected early?
Early-stage glaucoma often lacks noticeable symptoms. By the time patients notice their visual field narrowing, irreversible damage to the eyes has already occurred. Therefore, adults are advised to undergo comprehensive eye examinations every one to two years to monitor intraocular pressure, corneal health, and other ocular conditions, ensuring timely intervention before irreversible damage sets in.

有近視又有老花,LBV 激光矯視可以一次過解決?
有近視同老花並存,LBV(Laser Blended Vision)老花激光矯視可以一次矯正兩個問題?了解 LBV 雙眼景深融合原理、術前評估條件、適合人群及術後期望。

高度近視做白內障手術:晶體度數點計、視網膜點評估?
高度近視眼球軸長較長,白內障手術晶體度數計算需用進階方程式,視網膜脫落風險亦較高。了解術前須做哪些特殊評估、晶體選擇有何限制,以及手術後有機會減少眼鏡依賴。

Consultation Registration
